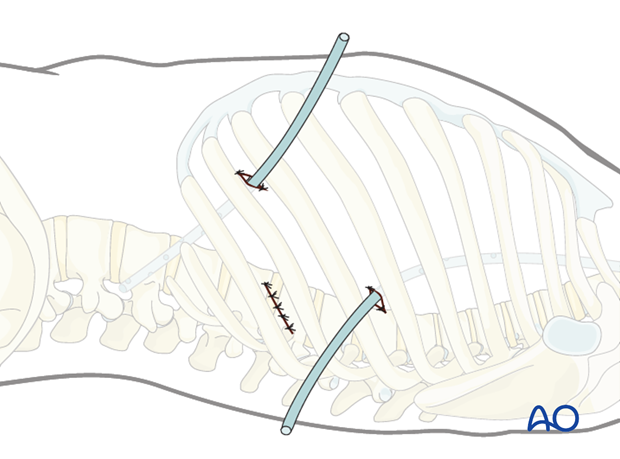
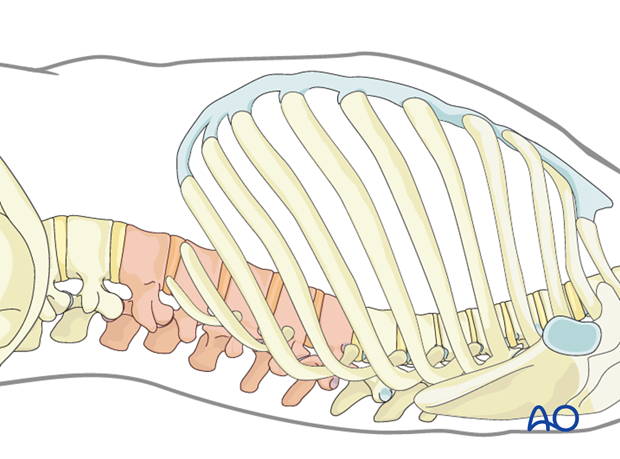
Minimally invasive left side thoracic approach
1. Portal site
The exact portal site will depend on the level of the fracture.
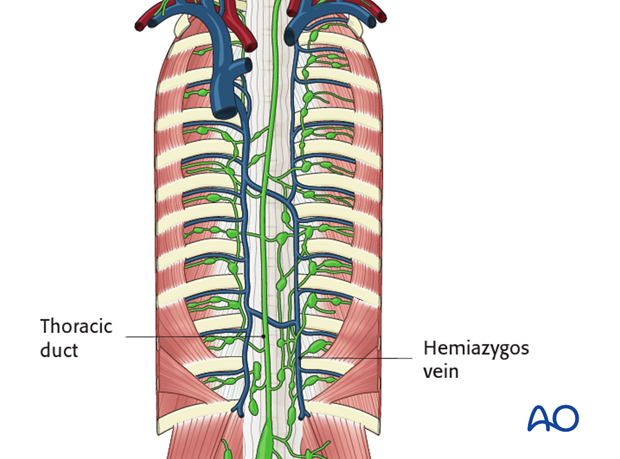
The approach can be made by the right or left side. On the right the surgeon will manage the thoracic duct and on the the left the hemiazigos vein might have to be ligated. The aorta is not of concern because it is shifted anteriorly to the apex of the deformity.
2. Preparation
Under fluoroscopic control, the apex of the deformity is located and marked on the skin of the left thoracic side
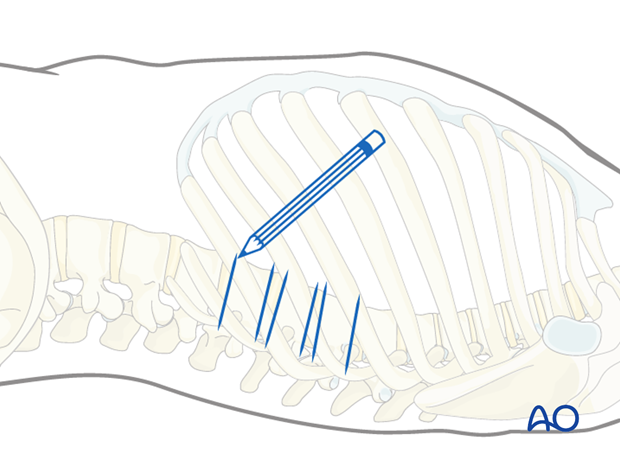
Usually the disc are close and a small incision centered on the apex of the deformity allows for anterior release of up to 5 discs.
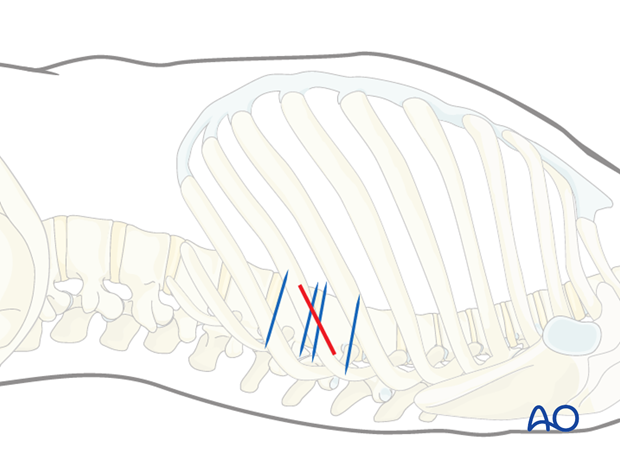
3. Minithoracotomy
The skin is incised on the mark.
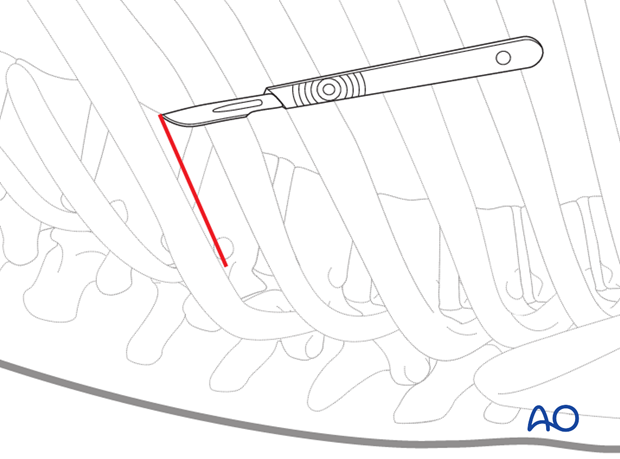
The skin and subcutaneous tissues and overlaying muscles are incised in line with the incision down to the rib to be exposed.
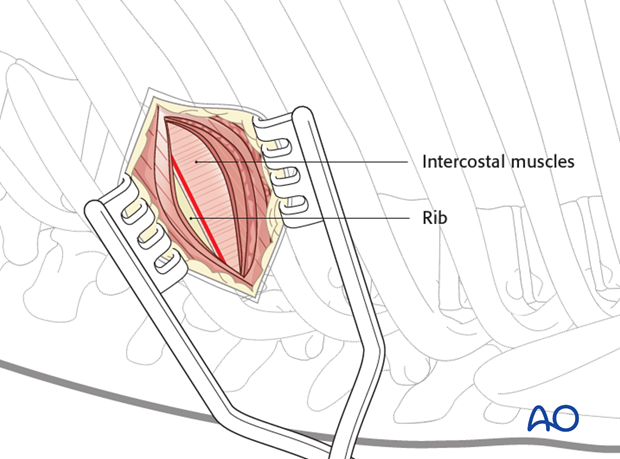
After exposing the rib, the intercostal muscles are dissected from the cranial part of the rib.
The pleura is then cut to allow entry into the chest without injuring the lung. A rib spreader can be used to gradually open the space created.
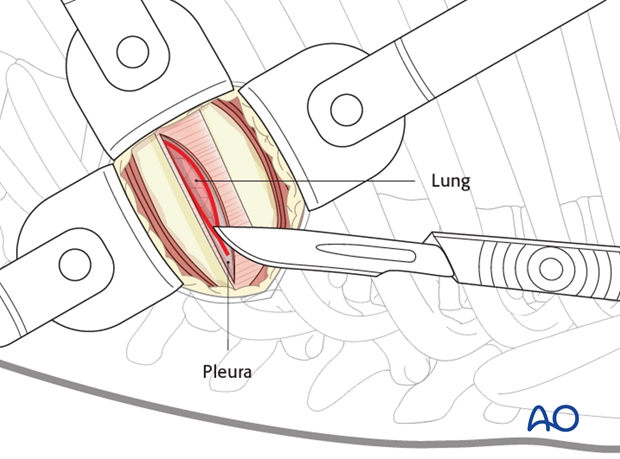
4. Additional portals
The thoracoscope is inserted through the minithoracotomy and a VAT is performed of the entire thorax.
This is done to examine the chest cavity for adhesions or anatomical variations prior to preparation of any further portals.
The other portals are placed under thoracoscopic control.
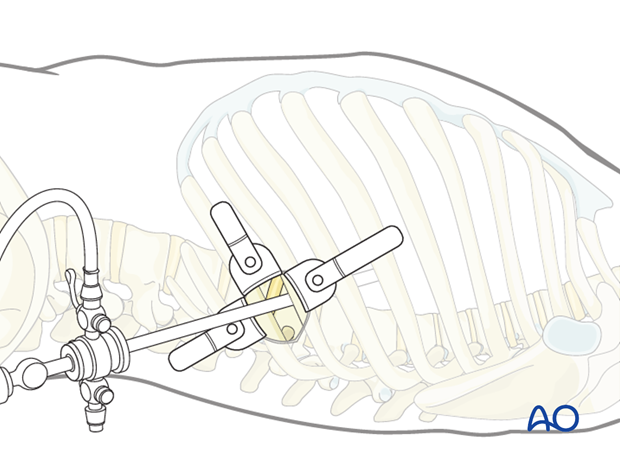
5. Portals
The viewing portal is marked first, two intercostal spaces cranial to the minithoracotomy at the anterior edge of the vertebral body.
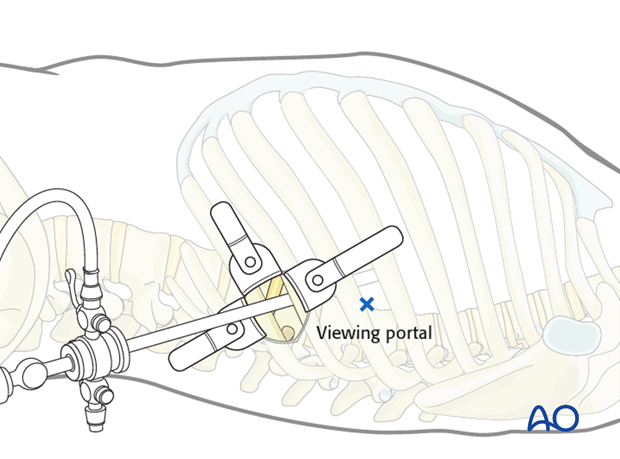
The retraction portal is marked one intercostal space cranial to the minithoracotomy and approximately 10 cm anteriorly.
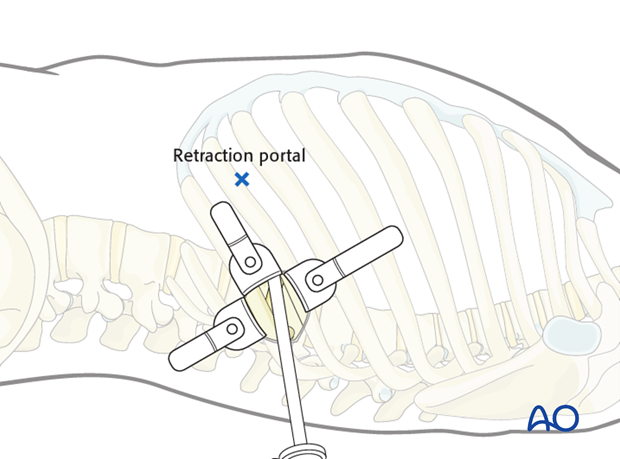
6. Incisions for the portals
A 20 mm skin incision is made for all portals. The incisions are deepened by sharp dissection to the pleural cavity at the upper rim of the rib to avoid injury to the intercostal vessel and a finger is introduced into the chest cavity to check for adhesions.
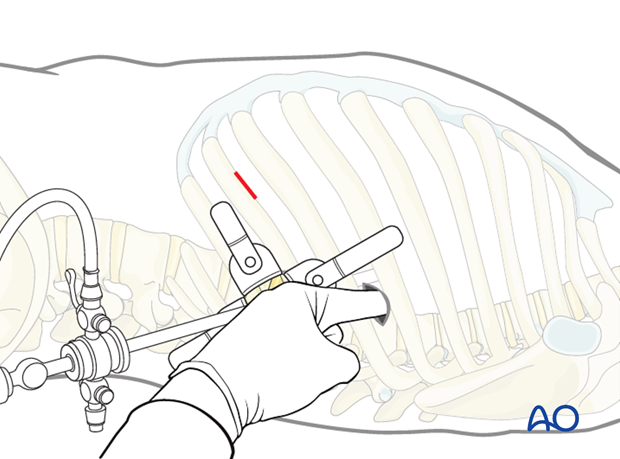
A blunt trocar is introduced under thoracoscopic control.
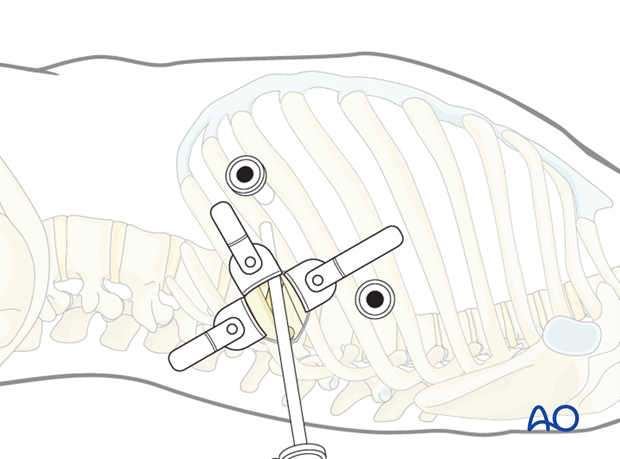
Now, the thoracoscope is retracted from the minithoracotomy and inserted into the viewing portal.
The retractor is inserted through the retractor portal.
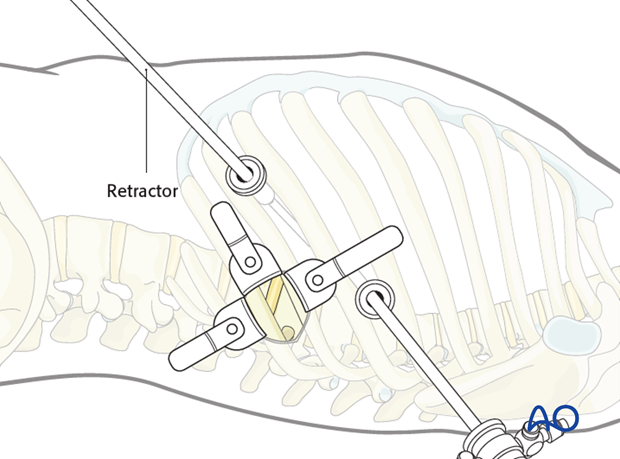
The self-retaining retractor system can now be used to expose the spine.
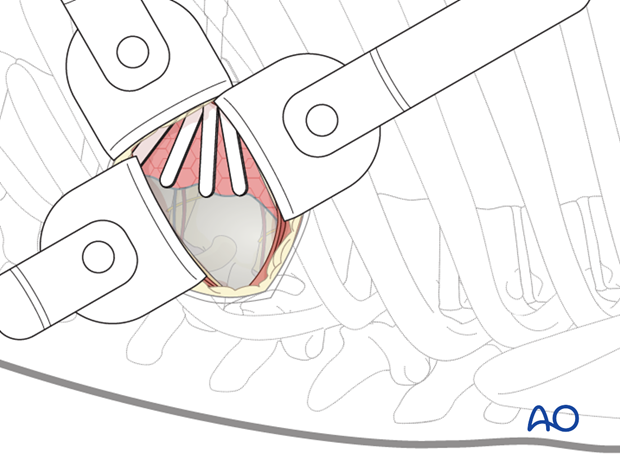
7. Instruments for miniopen and thoracoscopic approaches
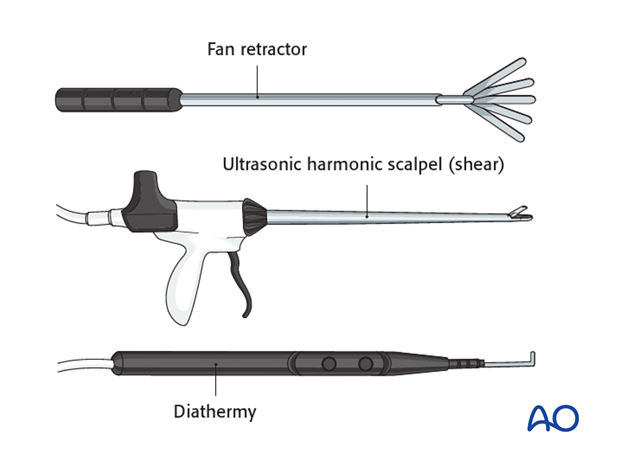
Specialized long instruments are needed for dissection. As an example, a fan retractor can be used to carefully hold the lung or diaphragm tissue away from the vertebrae.
An ultrasonic harmonic scalpel or shears are very useful tools for both cutting and coagulating tissues if available. An alternative would be a long hook shaped diathermy tip.
8. Further dissection
The parietal pleura should be opened longitudinally over the spine at the fracture level and a level above and below. It is easiest to begin the dissection at the discs, which will appear as avascular "hills". The "valleys" are the vertebral bodies, and the segmental vessels are in the midline.
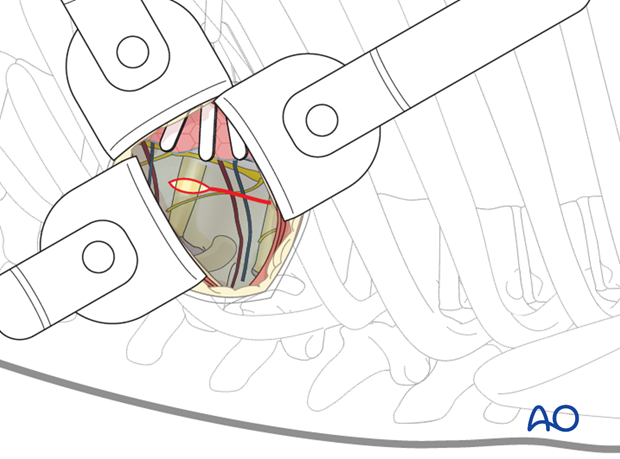
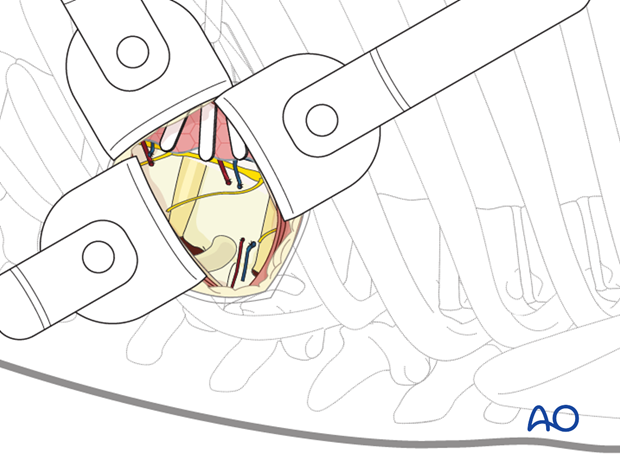
The segmental vessels running along the vertebral bodies are identified. For anterior discectomies, these can be spared. Attention should be payed to these vessels as they can cross the disc space due the angular deformity, and therefore need to be ligated.
A subperiosteal exposure is then undertaken to the level of the anterior longitudinal ligaments with protection of the great vessels. The ALL is usually thickened at this region and cutting it increase the release and posterior correction of the deformity.
Posteriorly the dissection should expose the heads of the ribs.
9. Closure
If possible, the parietal pleura should be sutured.
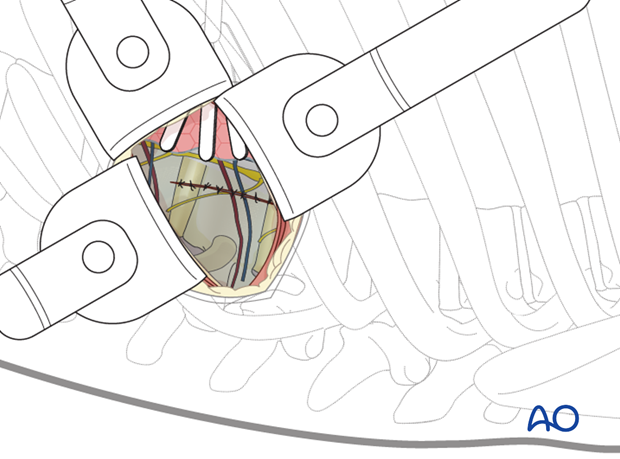
The viewing portal should be removed last to allow a direct inspection of the pleural cavity. The anesthesiologist should be asked to fully inflate the lung, which can be checked with the thoracoscope.
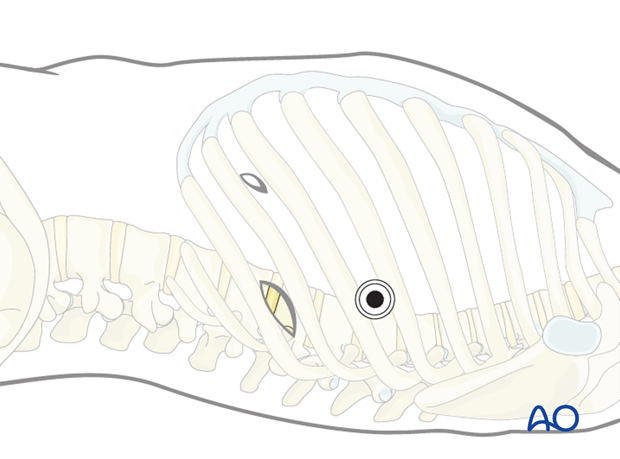
Two chest drains are then inserted. One via the viewing portal, which is directed to the cranial anterior part of the thoracic cavity (pneumothorax drain). The second one is placed in the retraction portal to the caudal posterior part of the thoracic cavity (wound drain).
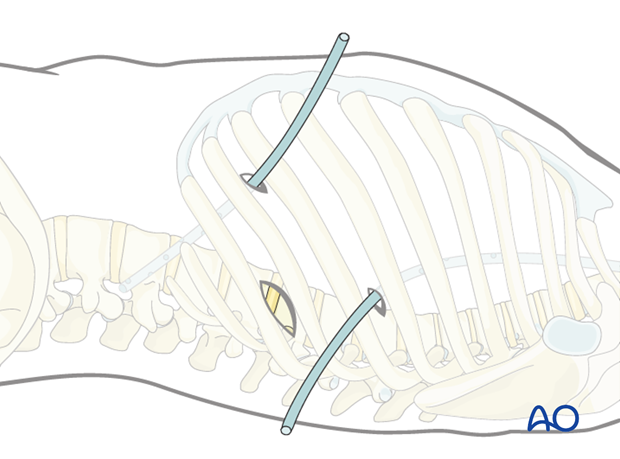
The portals and the minithoracotomy are then closed in layers.